Blood glucose (also called blood sugar) is a primary marker for determining diabetes risk. The higher your blood sugar, the higher your risk factors. But blood sugar is not just a marker for diabetes. As blood glucose levels rise, so does the risk for many other life-threatening conditions, most notably heart disease.
The best way to mitigate your risk is to keep your blood sugar levels at a normal range. What is the range for target blood sugar levels, you may wonder? The answer is controversial. The American Diabetes Association (ADA) delineates certain levels as “normal blood sugar levels,” but the ADA’s “normal” may not mean “optimal.”
What’s more, measuring blood glucose isn’t the only (or even the best) way to assess metabolic health. Many other biomarkers are also important. In this article, you’ll learn all about blood glucose: the basics, measurement, management, and what levels are considered healthy.
What Is Blood Glucose?
Glucose, as you’re probably aware, is a form of sugar. Alternatively, you can call glucose by its other name: carbohydrate. Yes, when you eat starchy carbs or sugar, you’re eating glucose. That glucose then passes through your gut and into your bloodstream.
The term “blood glucose” simply refers to sugar molecules (C6 H12 O6) floating around in your veins and arteries.
Blood glucose is necessary for survival. Your red blood cells, for example, can’t use any other fuel. And although your brain requires some glucose, even on a ketogenic diet, you don’t need to eat carbs to provide it.
When glucose is scarce (during a fast, for instance), your blood sugar doesn’t go down to zero. Instead, to keep glucose levels up, your body activates two glucose backup mechanisms:
Glycogenolysis: The release of stored glucose (glycogen) from muscle and liver cells.
Gluconeogenesis: When glycogen becomes depleted, your liver makes glucose from protein and lactate.
But in obese and diabetic populations, glucose isn’t scarce. Rather, there’s too much of it.
Blood Sugar, Insulin Resistance, and Disease
Within the past 30 to 40 years, there has been a dramatic increase in sugar consumption, which has been linked to rising rates of obesity and type 2 diabetes.
It’s a bit more nuanced, however, than more dietary sugar = high blood sugar = diabetes. We need to talk about insulin.
You see, when you eat a meal, your blood sugar rises, and your pancreas secretes the hormone insulin, which helps move that blood sugar out of your blood and safely into cells. Insulin acts like a good blood sugar boss, keeping your blood vessels safe from the dangers of hyperglycemia (elevated blood sugar levels).
But when sugar consistently enters the body (think daily Big Gulps), the boss gets overworked. And when the boss gets overworked, it can’t do its job anymore.
This is called insulin resistance – the inability of insulin to effectively store blood sugar in muscle and liver cells. In a state of insulin resistance, blood sugar stays too high for too long. This is how type 2 diabetes starts.
In addition to diabetes, insulin resistance and hyperinsulinemia (elevated blood insulin levels) underly many other chronic health conditions: heart disease, fatty liver disease, metabolic syndrome, and Alzheimer’s disease, to name just a few.
Later, you’ll learn strategies for preventing insulin resistance. But first, a word on measurement.
How To Measure Blood Glucose
To quantify your metabolic health, you’ll need to measure blood glucose levels. Common tests include:
- Hemoglobin A1c (HbA1c): Provides a rough “average blood glucose” estimate of the past 2-3 months by measuring the amount of sugar stored in red blood cells.
- OGTT: The oral glucose tolerance test (OGTT), administered in a lab, involves ingesting a sugary solution and measuring its impact on blood sugar levels at various timepoints.
- Fasting blood glucose: Your blood glucose after an overnight fast of around 12 hours.
- Postprandial blood glucose: Your post-meal blood glucose, which peaks 1 to 2 hours after eating.
Both fasting blood sugar and postprandial blood glucose are simple home blood tests, provided you have a glucose meter. Just prick your finger, insert the test strip, and record your result. If you have a Keto-Mojo blood glucose and ketone meter you can track your results over time with the free MyMojoHealth app.
Taking a blood sugar test is an ideal way to learn the effects of different foods on your body. Simply take a baseline reading (at least 3 hours after your last meal), eat a particular food, then test one or two hours after eating. You might be surprised which foods spike (or don’t spike) your blood sugar. See this guide to testing for your bioindividuality and learn which foods elevate your glucose levels so you can avoid them.
What Should Your Blood Glucose Levels Be?
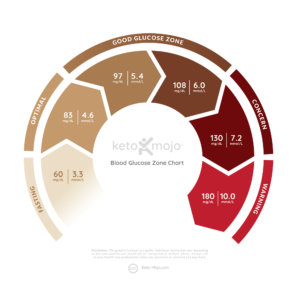
That is the question, isn’t it? To start, here’s how the ADA classifies diabetes based on fasting blood glucose (FBG) and hemoglobin A1c (HbA1c), which reflects average blood sugar levels over two to three months):
Normal: FBG under 100 mg/dl (5.6 mmol/L), HbA1c under 5.7%
Prediabetes: FBG from 100 to 125 mg/dl (5.6 to 6.9 mmol/L), HbA1c from 5.7% to 6.4%
Diabetes: FBG over 125 mg/dl (6.9 mmol/L), HbA1c 6.5% or above
But “normal” doesn’t necessarily mean “optimal.” Case in point: A large observational study following 46,578 people without diabetes over seven years found that those with FBG levels between 95 and 99 mg/dl (5.3 to 5.5 mmol/L) – considered normal – were 2.33 times more likely to develop diabetes than those with FBG levels below 85 mg/dl(4.7 mmol/L).
So, for fasting blood glucose, somewhere south of 85 mg/dl (4.7 mmol/L) seems best. But what about after eating?
As a general rule, the smaller and shorter the spike in blood sugar, the better. Practically, try to keep blood sugar spikes to less than 30 mg/dl over baseline at one hour post-meal. (If your baseline is 85 mg/dl (4.7 mmol/L), you don’t want to exceed 115 mg/dl (6.4 mmol/L). And by three hours after eating, you should be back near your baseline. This indicates that insulin — your blood-sugar boss — is doing its job.
A quick caveat on fasting blood sugar and postprandial blood glucose measurements: They’re not the most reliable measures of metabolic health. Stress, for instance, can cause the liver to secrete glucose into the bloodstream. If you’re nervous before the test, it could throw off the results. A poor night of sleep could have a similar effect. And then there’s the “dawn effect“, a natural release of cortisol in the early hours of the morning — which elevates glucose — to help your body get ready for rising. So, it’s best to wait an hour or more after waking to take your fasting blood glucose, and even longer if you have insulin resistance.
That’s why, in addition to measuring blood glucose levels, you should measure HbA1c and insulin levels. Measuring the insulin response following an oral glucose tolerance test (OGTT) can give insight into your metabolic flexibility. Often, a hyperinsulinemic (high insulin) response to glucose is a precursor for type 2 diabetes.
Also, measure your GKI — the ratio of glucose to ketones in your bloodstream — which can provide a more complete picture of metabolic health.
Managing Your Blood Glucose Levels
Here are some proven strategies for keeping blood sugar levels within a healthy range:
- Exercise: Both aerobic exercise and weight training have been shown to have positive effects on blood sugar, particularly when the two are combined.
- Fasting: Start with 16-hour intermittent fasts, and work your way up as your comfort and schedule permit.
- The ketogenic diet: The ketogenic diet minimizes carbs, helping minimize the blood sugar response (carbs are sugar, after all).
- Measure your blood glucose: Knowing how blood sugar fluctuates with different foods can help you make smarter choices.
- Sleep well: Sleep is crucial for maintaining good blood sugar control and insulin sensitivity. Prioritize it.
The Relationship Between Glucose and Ketones
Glucose and ketones tend to be inversely related. As glucose rises, ketones fall. But blood sugar responds more quickly to the introduction of foods than ketones do, which is why measuring glucose on a ketogenic diet is so important in sleuthing out foods that will adversely impact ketosis.
The Final Word
If you aren’t tracking your blood glucose, now is the time to start a blood sugar chart listing your test results. Along with other tests, it gives you an important picture of your metabolic health.
Optimal fasting blood sugar ranges are likely between 70 mg/dl and 85 mg/dl (3.9 and 4.7 mmol/L).
Measuring blood glucose is easy. You need only a glucometer (glucose monitor) and test strips. It’s an excellent tool to identify the foods that cause an elevated response in blood sugar in your body so you can adjust your diet accordingly.
To keep your blood sugar under control, be sure to exercise, sleep, and to keep carb intake low. To really kick it up a notch, follow a ketogenic lifestyle, with or without intermittent fasting. All these strategies enhance the function of insulin, which in turn improves your blood sugar response.
As always, before making dramatic diet and lifestyle changes for weight loss or other reasons, it’s important to discuss the idea with your healthcare provider, especially if you’re at higher risk for cardiovascular disease.


